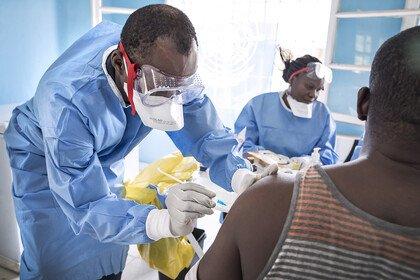
Learning from pandemics
Wellcome's Head of Prevention, Charlie Weller spoke to us about how the lessons of previous epidemics helped us respond to Covid-19.
Pressing play on the video above will set a third-party cookie. Please read our cookie policy for more information.
2020 and Covid really opened our eyes to the fact that a global pandemic is really a global problem and therefore it needs a global solution.
I was always interested in how things work. So, how the human body works, how cells work and so I was drawn to the sciences. And I studied the interaction between parasites and the immune system, how they live together.
I was really enjoying my work in academia, so I stayed on at Imperial College for 10 years. I moved into industry for a few years to support new drug development and antibodies. But again, that still was too far away from people. And then I looked at the Wellcome Trust, and this is really where society and science come together. And it was absolutely the right home for me.
I started at Wellcome in June 2014 and that was in the midst of the West African Ebola outbreak.
The process to develop vaccines is very long. It normally takes 10 years. And so there had been some work at an early stage in the lab to understand and to develop a vaccine for Ebola. But it hadn't got to the stage where it had been tested for safety in people. I think six weeks after I started, we, at Wellcome, decided to put a call out for clinical trials to assess vaccines and therapeutics, treatments that would impact the current outbreak.
We had to assess the safety of the vaccines, and only once we had the safety could we then move on to understanding if the vaccines could protect. You don't need to do the safety assessments in an outbreak. You can do that any time. So it delayed the time that we could assess for protection, which potentially cost lives.
But the one good thing about this whole process was there were many high-level reviews that were done following the Ebola outbreak on how this can be done better, what's more effective.
The World Health Organization (WHO) reorganised itself. They set up a more effective way to respond to outbreaks. They also incorporated research in the outbreak response, which is critical.
And the second big piece, to ensure that we never get into the situation again, that we have vaccines, but they haven't been safety tested, was the development of the organisation CEPI (the Coalition for Epidemic Preparedness Innovations), and its mission is to develop vaccines where there is market failure. To develop vaccines for those priority pathogens, those emerging infectious diseases, and Disease X – the unknown.
The Wellcome Global Monitor showed a couple of years ago that low-income countries, in general, had higher confidence and trust in the safety of vaccines than high-income countries, which stood out as one of the findings. And the obvious question is, why is this? Why would it be that high-income countries generally have less and lower confidence and trust in vaccines?
My interpretation would be that we in high-income countries are so fortunate to have vaccines that we have throughout our childhood for polio, measles, diphtheria. We don't see the disease. So we don't see it and we don't recognise it as being so devastating and therefore don't understand how valuable these vaccines are.
And then Covid comes along and reminds us all in 2020 of how devastating and how powerful infectious diseases are. They impact our communities. They impact and have devastating effects on our economies.
But also the flipside of that is we also understand and are reminded of the power of vaccines and human innovation to develop those vaccines, to repair those communities and to get our economy back on track.
What was seen in Covid – what was seen in 2020 – was the development of a vaccine within a year. That is unprecedented. A word that's been overused, but it really is. There are many reasons why we were able to move so quickly as a global vaccine community.
Firstly, we had certain systems in place. Organisations like CEPI, who were already working on coronaviruses, such as MERS and Disease X, and they could pivot their programs relatively quickly.
We also thought differently about how you conduct a clinical trial. So, a normal process involves a preclinical stage. Phase one clinical trials are on safety. Phase two looks at the different doses of vaccines, and phase three looks at whether the vaccine can protect. What was done in 2020 for Covid was in parallel. Manufacturing was started very, very early on at the same time as clinical studies, at financial risk. And that's not been done before.
There are many silver linings and many positives that have come out of the Covid pandemic.
We've got the mRNA vaccine validated now that's going to potentially open up a whole new era of vaccinology.
I think it also has opened our eyes to what we call vaccine nationalism and equitable access to vaccines and why it's so important for a global pandemic, you need a global solution. And that's really pushed us to think about how we can work more closely together.
But the one that always has stood out for me in Covid, but also in previous pandemics, is people's willingness to just try their hardest. To club together and really try and make a difference. And this I've really seen with the clinical studies, with researchers, industry, policymakers and the amazing volunteers that there are. Those healthcare workers who are making this happen. And that's always kind of the guiding light for me.
Covid is really the first global pandemic that any of us have lived through. Historically we have seen what's called a panic and neglect cycle when it comes to epidemics, and what I mean by that is when you're in the moment of an epidemic, all guns blazing, trying to solve the solution, but when it's calmed down, when it's gone away, your attention is diverted elsewhere. But for Covid and this global pandemic, I'm already seeing the preparedness and the discussions around preparedness for the future so that we can detect viruses and bacteria. So we've got the tools ready and poised to go. So we're that bit closer, that bit more prepared and we're looking out for the next pandemic, because with climate change and what we're seeing, epidemics and pandemics are only going to be more and more regular and in our lives.
About Charlie Weller
Charlie Weller has been at Wellcome since 2014. In September 2021 she became Head of Prevention in the Infectious Disease team, after five years leading the Vaccines programme at Wellcome to enable development of new and improved vaccines and the better use of vaccines. Her work at Wellcome has also included leading the development of our vaccines strategy, overseeing the funding response to the West African Ebola epidemic, helping to co-found CEPI, the Coalition for Epidemic Preparedness Innovations, and developing strategic thinking about future epidemic preparedness.
Before joining Wellcome, Charlie worked at Novartis as a lab head for respiratory exacerbations. She also worked at Imperial College London for eight years as Asthma UK post-doctoral Fellow. Charlie has a PhD in Biochemistry (Immunology) from Imperial College London and an MPhil and BSc in genetics from the University of Birmingham.
This interview was filmed in April 2021.

