How can the world adapt to Covid-19 in the long term?
Covid-19 is here to stay. However, with careful management we can prevent future outbreaks and move from pandemic to endemic. But what does this mean, and what must we do to stop it from erupting again?
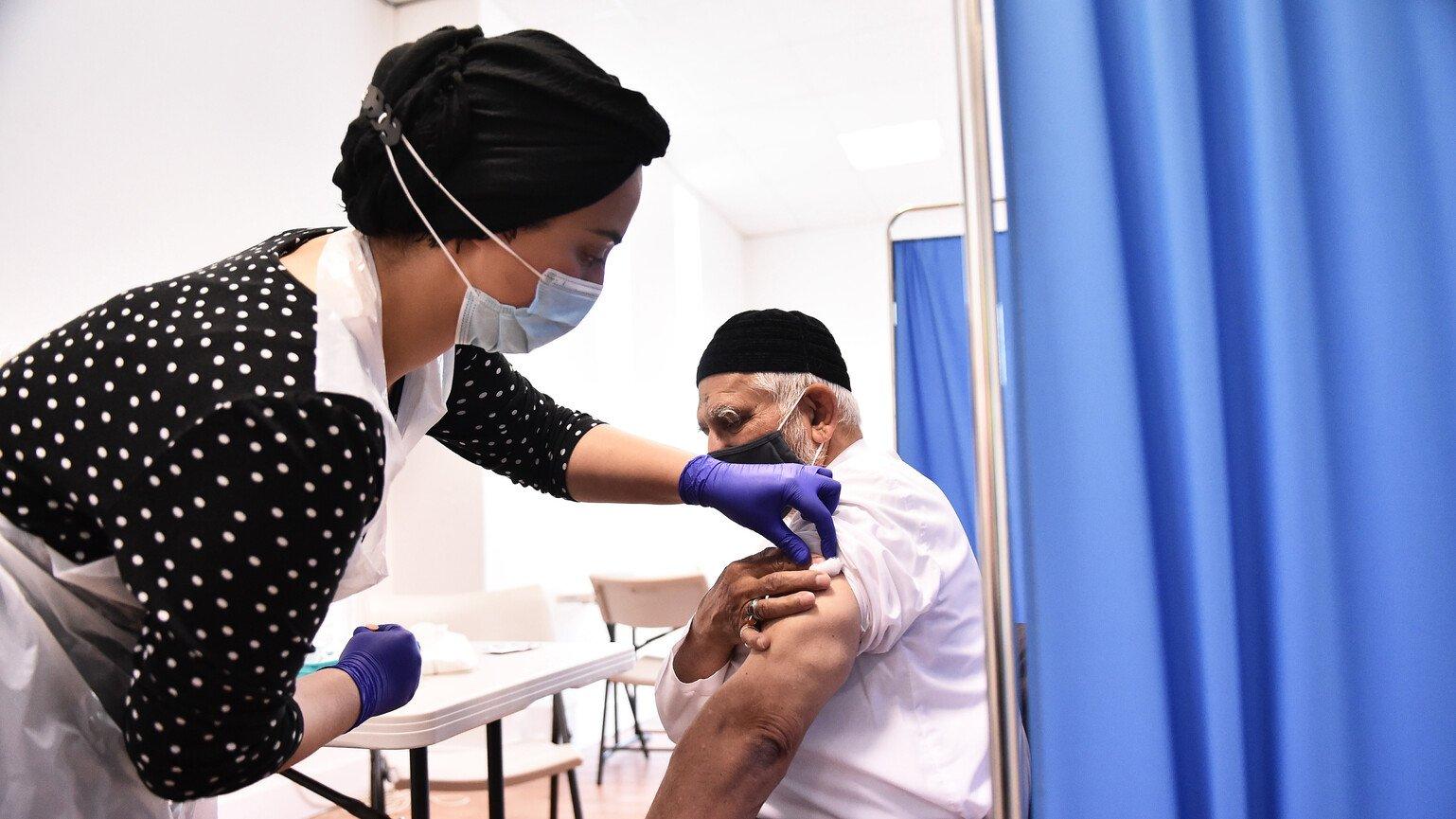
Nathan Stirk/Getty Images
Even with successful vaccination programmes, we can’t expect to completely eradicate Covid-19 from the world.
It will continue to circulate for many years to come.
Covid-19 is now established across almost the entire globe. Over time for most countries, it will change from an epidemic disease – where cases rise suddenly – to an endemic disease – where cases continue to appear long-term, with occasional peaks and troughs.
Click image to open gallery
Lots of diseases are endemic, ranging from relatively minor ones like the common cold viruses to major killers like malaria.
A disease can become endemic in a small region, like Lassa fever in parts of West Africa, or across the whole world, like chickenpox.
An infectious disease becomes endemic when it doesn’t spread so fast that it surges out of control, but at the same time it isn’t entirely eliminated. This might be because:
- we only develop limited immunity
- the disease spreads in ways we can’t fully prevent – for example through insect bites or when we breathe or talk, or
- the disease is established in wild animal populations where it can’t be wiped out.
In fact, the only human infectious disease that we have managed to completely eradicate is smallpox. This was a long and complicated process and required a global effort, helped by the facts that smallpox only infects humans (and not animals), it has a short incubation period, and we had a highly effective smallpox vaccine.
For most other diseases, full eradication is not feasible – we reduce their spread through measures like vaccination.
The prospects for post-pandemic Covid-19
This is what’s starting to happen to Covid-19 in countries that have had access to vaccines – like the UK, Germany and the USA.
People are increasingly building up immunity through a combination of vaccinations, booster doses and the natural immunity that people develop after infection. However, where vaccines haven’t been available there are lower levels of protection against the virus.
The longer this virus continues to spread in largely unvaccinated populations, the more likely it is to evolve and produce new variants like Omicron or Delta. These might spread faster or make people more seriously ill – and may even reduce the effectiveness of our current vaccines.
If we can increase global immunity, this will make it harder for the coronavirus to spread.
We may then get to a point where countries regularly have only a small number of Covid-19 cases – that might feel like mission accomplished. But there will still be work to do to keep ourselves protected.
An example of major outbreaks starting again, after a disease had been brought under control, is measles in 2018. Vaccination uptake had dropped in several countries, which reduced herd immunity below the threshold that kept the disease in check, and cases surged to an estimated 10 million worldwide.
So, what can we do to manage Covid-19 in the future?
This pandemic is not yet under control and there’s still a lot we don’t know about Covid-19, including how long a person’s current immunity might last and the impact existing and future variants may have.
But we do already know what the world’s long-term anti-Covid-19 plan has to involve:
- Monitoring the virus. Knowledge is power, and a global programme of genomic surveillance, coupled with other epidemiological and clinical data, will tell us when and where the virus is spreading and how it is evolving. Let’s not get taken by surprise again.
- Investing in vaccines and treatments. If new variants, such as Omicron or Delta, appear that behave more dangerously, we need to be ready to find ways to prevent their spread, to treat people who do get infected, and to reduce the overall impact on healthcare systems and societies.
- Ensuring that everyone in the world can access vaccines, treatments and tests. If we have learned one thing over the last two years, it’s this: an infection anywhere is a threat everywhere. The more people who have Covid-19, the more chances the virus has to evolve and spread. This means that controlling the virus in any one country will benefit people in every other country.
- Sharing and coordinating resources. Many countries lack the means to implement effective vaccination programmes. Out of solidarity and out of self-interest, richer countries need to invest in the ACT-Accelerator, a global collaboration working to ensure everyone, everywhere can access tests, treatments and vaccines. Rich countries that have secured lots of excess vaccine doses can also donate these through COVAX, which will ensure that vaccines go where they are needed most.
- Global solidarity. Acting in national self-interest will only ever perpetuate this crisis, trapping us in a cycle of waves, new variants, lost lives and continued economic and societal disruption. Clear and rational political decision-making, communication and global collaboration is crucial if we want to see the pandemic end.
We’re funding research to better understand what causes and drives infectious diseases to escalate and the solutions to control their impact. Explore our current funding calls:
Infectious Disease Clinical Trial Award: Optimising interventions for impact
This explainer was originally published in July 2021.

