Four lessons from past epidemics to guide us in the search for Covid-19 treatments
Even the deadliest viruses – like Ebola and HIV – can be made treatable, if we concentrate our efforts on research, development and access. With more than 200 potential Covid-19 treatments currently being explored in studies worldwide, what lessons can we learn from other epidemics about the development and use of treatments?
1. Treatments can turn the tide against epidemics, whether or not there’s a vaccine
When the first case of HIV was diagnosed in the early 1980s, science had no answers. There were no treatments or vaccines, and the epidemic went on to infect and kill millions of people worldwide.
Today there is still no vaccine. But, together with the right care, modern antiretroviral treatments can now suppress HIV to the point that it has no impact on life expectancy, reducing virus levels so low that the infection is untransmittable. Thanks to these treatments, people with HIV can live long, healthy lives.
And for diseases where a vaccine is available, treatments are still vital for saving the lives of people who haven’t been immunised.
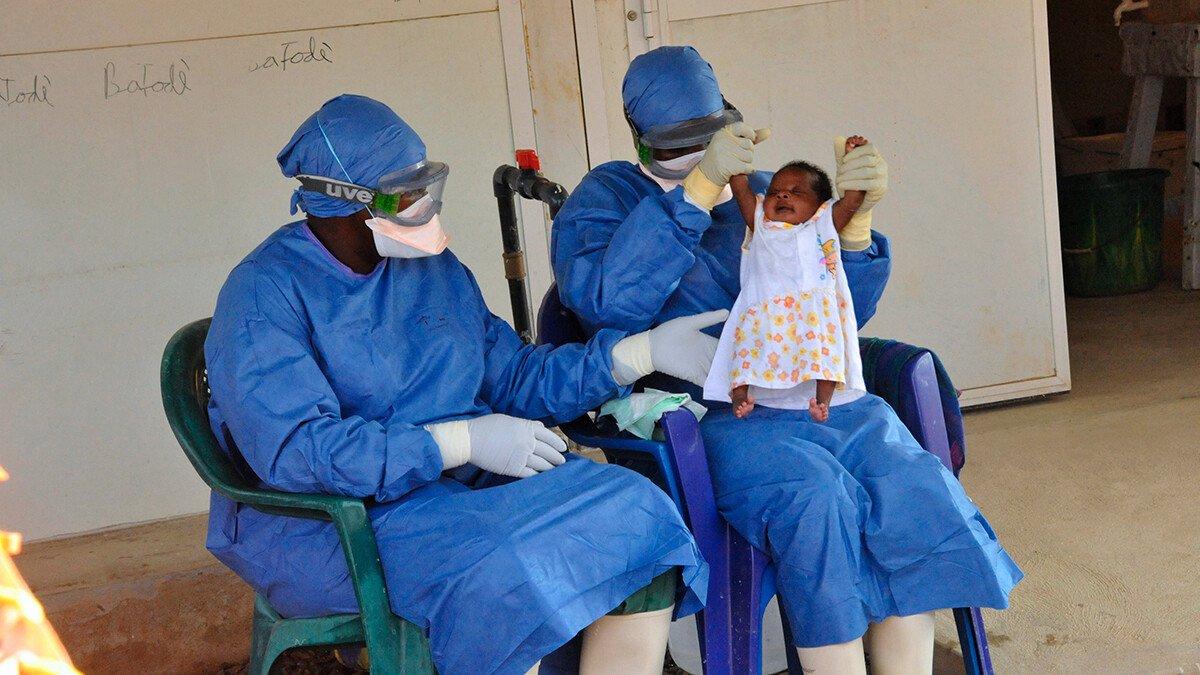
Outbreaks of Ebola, with a survival rate of around 50%, have taken thousands of lives and have had a devastating impact across West Africa. In 2019, clinical trials identified two treatments that worked well, and thanks to these drugs, more than 90% of infected people now survive if treated early. A vaccine has also been developed, but the treatments remain essential for those who have not been able to have it, whether for medical or economic reasons.
To make similar lifesaving progress against Covid-19, we must direct the same energy towards finding treatments.
2. Treatments must be available to everyone and work everywhere
The solution to this pandemic has to be global, so treatments must be accessible and affordable for everyone who needs them.
In the late 1990s and early 2000s, affordability was a major problem with the antiretroviral drugs for HIV. Treatment cost around $10-15,000 per person per year, until a movement by activists and NGOs led to competition from cheaper generic versions of the treatments. This brought prices down to $140 per person per year by 2005, paving the way for 22 million people living with HIV/AIDS to be able to access treatments by 2018.
But access is not just about pricing. It also means making sure that the treatment is appropriate for use in the places where it is needed, and that there is enough of it to meet global demand.
This is why the recent findings from the RECOVERY trial, showing that the steroid treatment dexamethasone can save lives from Covid-19, is so important. Dexamethasone is a low-cost drug that is already widely available and easy to manufacture worldwide. In many African countries, for example, the drug costs less than $2.
To tackle Covid-19 and make sure that access to new treatments is considered at the very start of the research and development process, governments and health organisations have come together through the ACT Accelerator – a global collaboration to support equitable access to all vaccines, treatments and tests that will help protect people against the disease.
3. Finding a treatment quickly relies on global coordination
Defeating Covid-19 requires global collaboration and pooling resources on everything from research infrastructure and funding to long-term planning. This is not something that one research team, one company or even one country can solve alone.
We’ve seen what can be achieved with global collective action – for example through global health partnerships like UNITAID and the Global Fund to fight HIV/AIDS, TB and Malaria. Through these, governments, NGOs, public and private sector organisations have come together to finance and scale up access to innovations, including treatments.
Since 2002, the number of deaths caused by AIDS, TB and malaria has been reduced by 40% in the countries where the Global Fund invests – showing the massive impact that collective action can make.
We need to continue to build on these partnerships, which is why the establishment of the COVID-19 Therapeutics Accelerator – a large-scale collaboration to research, develop and make Covid-19 treatments available – is so important.
It is only by coordinating and funding large trials in parallel that we will find game-changing treatments for Covid-19. The Therapeutics Accelerator is helping us get there by evaluating existing drugs and creating platforms for exploring new potential treatments. But it still needs much more funding.
4. We must be prepared for the next epidemic
The global response to Covid-19 has been unprecedented – a cause for great optimism as long as this effort can be maintained. But the world has been through enough epidemics for us to know by now that it’s better to prepare in advance.
There are many other diseases – including Lassa, Mers, Nipah, Marburg and Dengue – with potential to become widespread epidemics. We must be ready to tackle them, and to rapidly test and develop treatments and vaccines.
Part of this preparedness involves making sure that the research infrastructure is in place – for example that clinical trials to test treatments can be set up quickly. This is something that has been unprecedented for Covid-19, with the World Health Organization’s Solidarity clinical trial and the UK’s RECOVERY trial set up in record time.
If we don’t build on the successes of the Covid-19 response, and fund research and development related to likely future epidemics so we can test new drugs and vaccines swiftly during epidemics, we will remain vulnerable to outbreaks. We need to stop waiting for the worst to happen before we respond.


