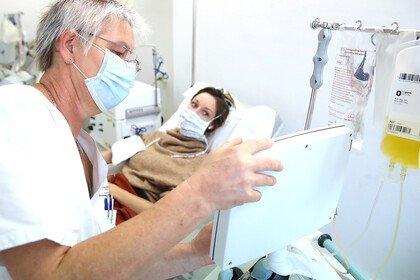
We need Covid-19 treatments as well as vaccines – and they have to work for everyone
Effective treatments, that are accessible to everyone who needs them, have to be part of the solution to the coronavirus pandemic – here's why.
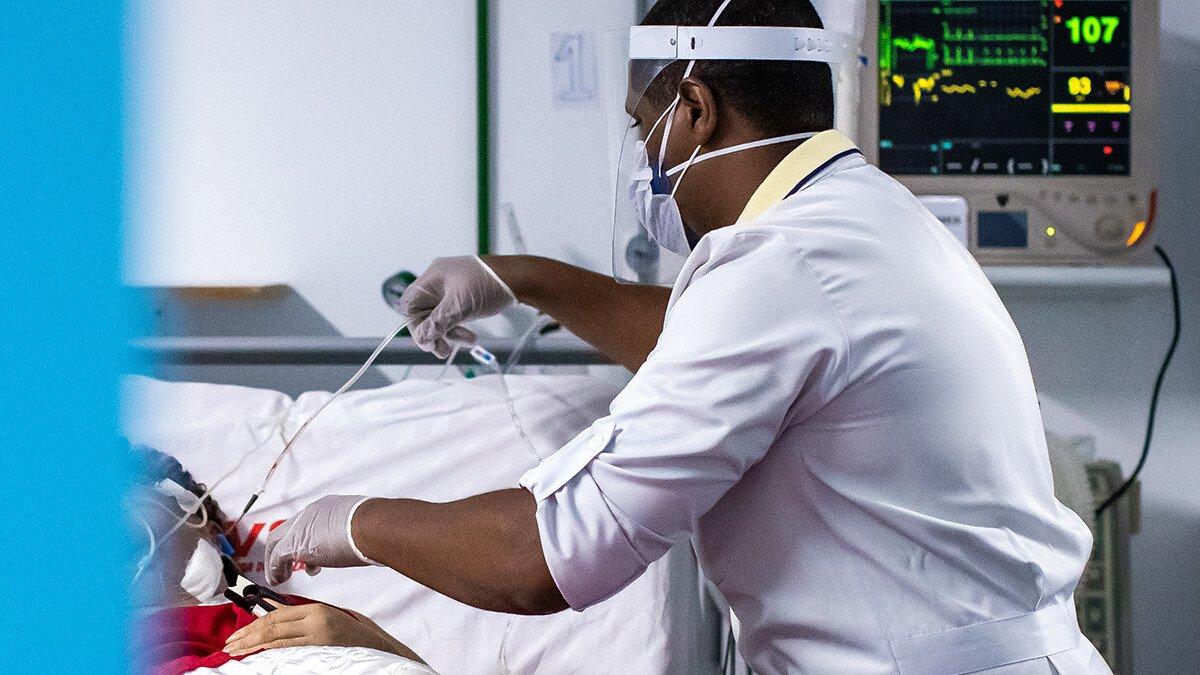
Our exit strategy from the Covid-19 pandemic relies on investing in research. But finding a vaccine won’t be enough – effective treatments have to be part of the strategy, too. And they must be accessible to everyone, everywhere – starting with those who need them most.
Treatments need to be part of the solution, too
A successful vaccine against Covid-19 would be a great lifesaving advance. But vaccines alone won’t be enough to bring the crisis under control.
Thousands of people are still becoming infected with the SARS-CoV-2 virus every day. Those who develop a severe illness can’t just wait for a vaccine to be developed, manufactured and rolled out – we need to invest in potential treatments now.
Vaccines are slow to develop and test. Researchers need to wait to see participants in clinical trials not becoming infected – and that takes time. By contrast, scientists testing treatments can observe infected patients in real time, directly seeing what works and what doesn’t.
In the space of a few months, researchers have found that hydroxychloroquine, remdesivir, lopinavir/ritonavir and interferon did not reduce the risk of dying of Covid-19 or the duration of hospital stay. So far, dexamethasone is the only drug which was shown to reduce mortality in hospitalised patients. Early clinical trial results for monoclonal antibodies have also been published, showing encouraging signs – researchers are hoping to know whether these new drugs are effective by the end of the year.
These quick results mean that, when knowing what doesn’t work, researchers and resources can be redeployed to look into other, more promising treatments. And, when finding treatments that do work, these can then be put into use to save lives.
"Treatments are not just a contingency for when the vaccine comes along."
Even when effective vaccines are found, the process of manufacturing and distributing them around the world will be complex. Nick Cammack, Wellcome’s COVID-19 Therapeutics Accelerator Lead, says: "Imagine we find a successful vaccine – one that develops the appropriate immunity – by the end of this year. It will still take a number of years to roll that vaccine out around the world." Effective treatments will help us save lives while this is happening.
Nor are treatments just a temporary solution – they're an integral part of how we tackle Covid-19. Even when we have a vaccine, people will continue to be infected. We also don’t know how much immunity it will give us, or for how long. For as long as people continue to get sick with Covid-19, we need effective treatments to help them. "Treatments are not just a contingency for when the vaccine comes along," says Nick.
Pressing play on the video above will set a third-party cookie. Please read our cookie policy for more information.
Watch Nick Cammack, COVID-19 Therapeutics Accelerator Lead, explain more about potential treatments.
The coronavirus that causes COVID-19 is a completely new virus, and we know very little about it.
Researchers are taking a wide range of approaches to find an effective and safe treatment. The three main approaches are antivirals, antibodies specific to the virus, and anti-inflammatory drugs.
Antivirals work by preventing the virus from replicating inside the body. It would be great to have an antiviral specific to COVID-19, but discovering one could take years.
In the meantime, researchers are hoping that antivirals used against some existing viral diseases might have some benefit in COVID-19.
Antibodies attack the virus directly. They are naturally produced by people who have had the infection and recovered.
When given to patients who are struggling to fight off the infection, antibodies can boost the immune response and inhibit the virus from replicating.
In patients with severe COVID-19, what actually happens is an exaggerated immune response aimed at clearing the infection.
We hope to use anti-inflammatory drugs to modulate that reaction, helping to clear the infection without causing any undue harm to the individual.
The solution must be global
Good science to produce treatments, tests and vaccines is crucial – and it can’t be confined to a few countries. A coordinated effort around the world will allow us to develop treatments that are a genuine global public good.
Producing effective treatments isn’t as simple as just finding a drug that works. Different treatments might have different effects in different settings.
"Populations vary," explains Trudie Lang, Professor of Global Health at the University of Oxford. "We expect to see differences from things like co-infections and what else is going on in the community. That might cause a difference in how people respond to drugs, but also what drugs you can use in those settings."
Pressing play on the video above will set a third-party cookie. Please read our cookie policy for more information.
There isn't going to be a single 'cure' for Covid-19.
That's because the virus affects us all in different ways, ranging from mild symptoms to life threatening illness and 'long Covid’.
So we need to develop different treatments.
Monoclonal antibodies could prevent severe disease, if given early, and antivirals could help hospitalised patients recover faster.
What’s more, all our bodies are different, so what works for one person might be useless or even harmful for another.
And different healthcare systems around the world need treatments they can deliver with the means they have to give us all the best chance of beating Covid-19.
We have to keep researching different treatment approaches and we need more funding for the scientists doing this work.
Find out more at wellcome.org/covid-19.
Differences don’t stop at the biochemical level – drugs against Covid-19 also have to be usable by local healthcare systems wherever they’re needed. "Clinical care settings are different as well," says Trudie. "The ability to test is very different... it does play into where people present with diseases and how they’re cared for."
So, at every stage of research and development, we need to find out what works for different communities to make sure the solutions to the pandemic are globally effective and equitable.
Wellcome’s recent funding call for Covid-19 focused specifically on interventions in low- and middle-income countries. Funded projects include studies in Kenya, Uganda and The Gambia. Research like this, on how the virus operates in different settings and the impact of interventions including treatments in those settings, will help us make sure we have drugs that are suitable for use in different communities around the world.
And that’s vital. Separate, national responses won’t work against a virus that doesn’t recognise borders. It will take a global effort to solve a global crisis. Successful drugs against Covid-19 – wherever they’re developed – must be distributed equitably around the world, starting with the places that need them most urgently. If not, the virus can never be brought under control.
"Until we have reliable tests to detect, medicines to treat, vaccines to prevent, the disease will keep going round the world in waves," explains Nick Cammack. "As long as it’s out of control somewhere, it’s always going to be a threat everywhere."
This article was originally published in June 2020 and updated on 19 October 2020.

