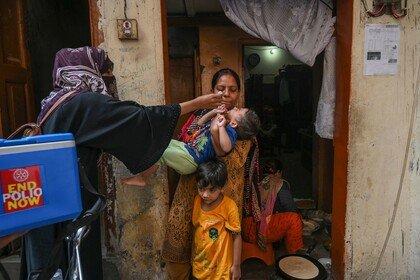How can we prevent epidemics? This initiative aims to find out
To prevent future epidemics and improve the response to ones that are already happening, there needs to be evidence, knowledge and the right tools. The Joint Initiative on Research in Epidemic Preparedness and Response (JIREP) aims to help provide these.

The Joint Initiative on Research in Epidemic Preparedness and Response is a collaboration between Wellcome and the Foreign, Commonwealth and Development Office (FCDO). The five-year initiative began in 2018 and is funding research around the world, facilitating collaboration and influencing policy change. It aims to do this across four issues that are crucial to combating epidemics.
With each project the Joint Initiative on Research in Epidemic Preparedness and Response supports, we’re getting better at doing so.
1. Prevent and manage outbreaks of known diseases
Many diseases with the potential to become epidemics keep coming back, for example Ebola and Lassa fever. Cholera is another one, and hits the poorest and most marginalised communities hardest. But deaths from cholera are preventable with the tools we already have. So what’s missing?
The World Health Organization (WHO) has set out a roadmap to reduce deaths from cholera by 90% by 2030. For this to happen, critical research evidence is needed to direct how best to use existing tools, and to develop new and better ones.
Through a targeted Joint Initiative on Research in Epidemic Preparedness and Response funding scheme, we’re supporting researchers to look at how to respond most effectively to outbreaks. For example, we’re funding a team at Fred Hutchinson Cancer Research Center in Seattle, USA, to investigate how best to use limited oral vaccine supplies to protect more people.
But vaccination strategies alone are not enough to control outbreaks.
To help boost prevention, researchers with the Ghana Red Cross Society will evaluate ways to improve water, sanitation and hygiene. And researchers with the Yemen Relief and Reconstruction Foundation will look at what lessons can be learned from the response to cholera in a conflict area.
"Yemen is experiencing the largest cholera/acute watery diarrhoea epidemic in recent history, with an estimated 1.4 million suspected cases. We hope that our research approach will allow us to identify the challenges at multiple levels − individual, social, community, health system and structural − that impact the ability of the population to benefit from cholera/acute watery diarrhoea control and prevention strategies."
2. Support affected countries to be better prepared for outbreaks
Infectious diseases can jump borders, but the country at the epicentre of an outbreak needs to lead the research and response strategies for these to be effective. International collaboration and expertise should help to build that local capacity.
This is why we’ve supported the African coaLition for Epidemic Research, Response and Training (ALERRT) to help strengthen research response to epidemics in countries across sub-Saharan Africa.
In the Democratic Republic of the Congo, an Ebola clinical trial on therapeutics – a breakthrough in the fight against Ebola – was rolled out last year. Through the African coaLition for Epidemic Research, Response and Training, Institut National de Recherche Biomédicale in Kinshasa is helping deliver local training to make the trial happen.
Nigeria faced the largest Lassa fever outbreak last year. With support from the Joint Initiative on Research in Epidemic Preparedness and Response, the African coaLition for Epidemic Research, Response and Training is helping to support clinical research in the country, and the WHO is strengthening the country’s research response.
3. Integrate social science research in epidemics response
Understanding issues around practices, beliefs or geo-politics are crucial to prevent and control disease outbreaks. Social science research needs to be integrated in epidemic responses and we want to help that happen.
Through the Joint Initiative on Research in Epidemic Preparedness and Response we’ve supported researchers at the Social Science in Humanitarian Action Platform to develop a network of social science advisers in the areas affected by the Ebola outbreak. They’ve been shaping the epidemics response on the ground with evidence-based timely briefings.
4. Link evidence with policy
Ultimately, research creates evidence about what works or could work – and for this evidence to be put into practice, it needs to reach national, regional and global policy makers.
Through the projects we fund, we want to create more evidence that translates into better policies.
The Brazilian Ministry of Health launched a massive yellow fever vaccination campaign in 2018 using fractional dosing, based on research evidence that this approach works. It means that when an outbreak occurs, more people can be protected using a limited supply of vaccine. One of the research projects we funded – led by Fiocruz in Brazil – showed that fractional dosing of the yellow fever vaccine can provide longer lasting immunity than was previously known.
Through the Joint Initiative on Research in Epidemic Preparedness and Response we want to support more collaborative research across the world. But as the threat of epidemics continues to grow, funders, governments and international organisations need to work together as a global community.