
Why are we seeing spikes in measles compared to other infectious diseases?
Last year we saw worldwide spikes in measles, largely due to sharp increases in just 10 countries. It seems that we hear a lot about measles compared to other infectious diseases, such as rubella or whooping cough. But why?
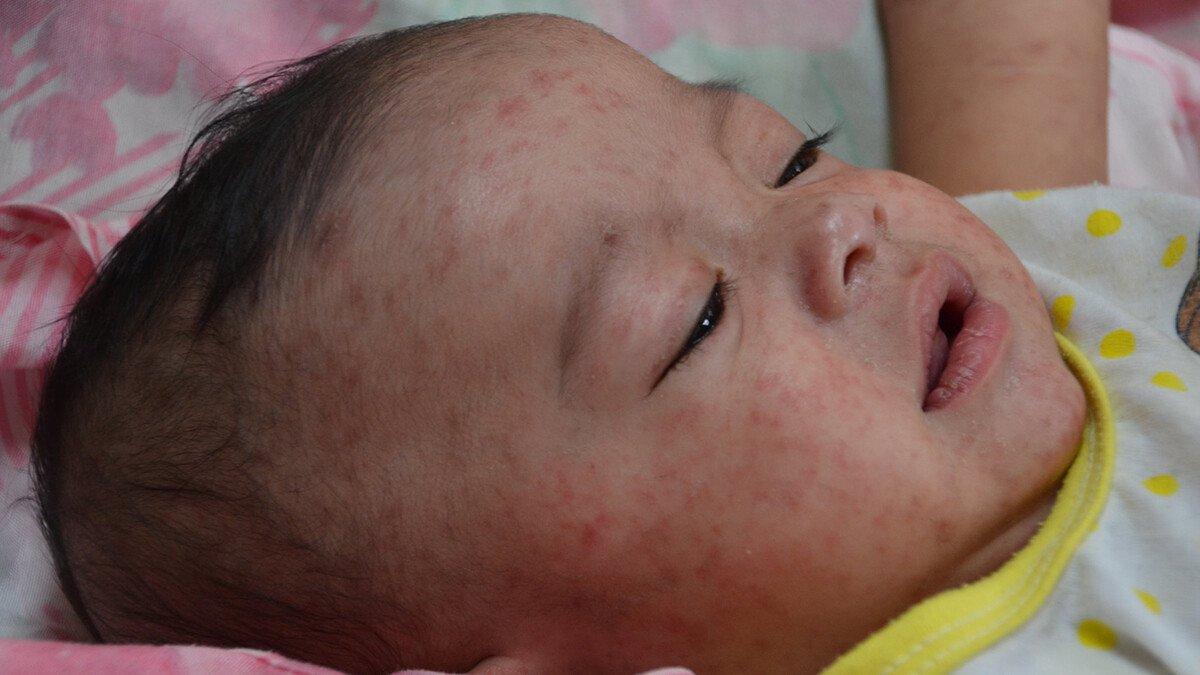
Measles is one of the most contagious infectious diseases in the world. On average, each person with measles would infect 12–18 other people in a totally susceptible population, ie one with no vaccine coverage.
When a disease is as infectious as measles, higher proportions of the population must be immunised to ensure herd immunity to protect those who cannot benefit from the vaccine.
With measles, 90-95% coverage is required to achieve herd immunity. So when vaccine coverage rates drop below this very high level, we start to see measles outbreaks. So we can think of measles outbreaks as a sort of early warning system for reduced vaccine uptake and global ‘canary in the coal mine’ signalling where there may be further or different outbreaks to come.
In July 2019, WHO and UNICEF jointly published the 2018 annual national immunisation coverage estimates for member states. Three things stood out to me:
- vaccine coverage rates have stagnated over the last decade
- most unvaccinated children live in the poorest countries, and are disproportionately in fragile or conflict-affected states
- with national statistics being reported, the local and regional situation isn’t being seen.
So why does this matter? For diseases where herd immunity is so critical to achieving effective vaccine coverage, such as for measles, the sub-national and even community level coverage rates are critical to maintain at a high level.
These local pockets of lower coverage are where measles outbreaks are likely to occur within all countries of all income levels, including those that have high national vaccination rates.
We should celebrate that nearly 9 out of 10 children worldwide are able to access and gain the benefits of vaccines, more than ever before. However, this is not enough. Coverage rates have only increased by 5% in the last decade. Why is this? While there have been increases in coverage rates in some countries such as India, we are seeing other countries backslide.
This is a complex situation with multiple causes that include:
- complacency that vaccines are not that important or relevant in our modern world
- lack of investment in public health
- conflict
- forced migration or fleeing home countries
- an inability to access health facilities
- in some places, lack of trust in the safety and effectiveness of vaccines.
A recent global report that surveyed 140 countries and more than 140,000 people showed that despite the overwhelming global majority of people agreeing that vaccines are safe and effective, there remain pockets where vaccine confidence is a real issue and may be playing a small but important part in stopping essential coverage.
We know vaccines are one of, if not the most successful public health interventions of all time, so how can we ensure that all people are able to enjoy the benefits they provide?


