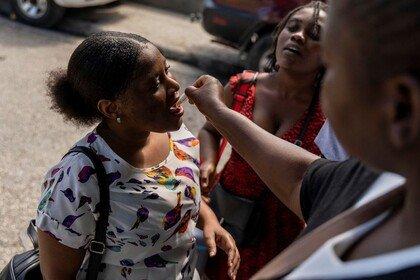
Childhood immunisation is recovering, but there’s a long way to go
20.5 million children hadn’t received essential vaccinations in 2022, according to the latest data from the World Health Organization (WHO) and UNICEF. While that marks an improvement to 2021, coverage still falls short of pre-pandemic levels for many countries.

WHO / Henitsoa Rafalia
This article was first published on 25 July 2022.
The data for immunisation coverage in 2021 and 2022 show in sobering detail what happens when an infectious disease like Covid-19 is not controlled or contained and escalates out of control on a global scale.
This is an important reminder that we must shift from responding to outbreaks when they happen to prevention. One reason why is that outbreaks like Covid-19 have a much wider impact on critical health systems. While routine childhood immunisation rates have started to recover from the impacts of the Covid-19 pandemic, there is a long way to go to vaccinate and protect children everywhere.
We can look to the cracks and challenges that existed before the pandemic to guide us on how to prevent disease escalation.
How do we prevent disease escalation?
Three key messages jumped out to me from reading the latest immunisation coverage rates.
1. We need global collective action on infectious disease
Immunisation rates are slowly recovering at a global level. However, the lowest-income countries remain extremely vulnerable. Coverage in Africa in particular is still lower than 2019 because of challenges such as lack of access to services.
Just ten countries account for the six in ten children who miss out on access to all life-saving vaccines. Roughly the same countries also account for six in ten of the children missing out on a measles vaccine.
The risk of outbreaks from diseases like yellow fever and measles remains high because of the huge numbers of children missing out on vaccination. This can create dangerous conditions for deadly diseases to escalate. For vaccines to work, coverage must be high.
In 2023, a new global initiative ‘The Big Catch-up' was launched to help do just that. A collaboration between Gavi, The Bill & Melinda Gates Foundation, WHO, UNICEF, and many other IA2030 partners, it aims to restore and strengthen routine immunisation in countries most affected by the Covid-19 pandemic.
2. We need to act early, predict and prevent
Measles is often described as ‘the canary in the coal-mine’.
It’s the first outbreak we see when immunisation rates are low and an indication of dangerous things to come. Measles outbreaks come first because it’s so infectious and measles vaccines need very high coverage to be effective.
While action was taken when Covid-19 infections rose above an R-rate of 1, measles has a staggering R rate of 12-18. That means an average of 15 people are infected from just one case.
In 2022, measles vaccine coverage remained below the 95% critical threshold and worsened in many countries around the world. With a drop in coverage and outbreaks spreading, measles is offering a warning sign that we need to take action. But waiting for outbreaks to begin isn’t the best way to protect the most lives and keep infectious disease under control.
For prediction and prevention to work best, we need strong, robust global surveillance systems with the capacity to measure and map the sources and drivers for all infectious diseases. We also need to use the best technologies – from genomic surveillance to citizen-generated data.
3. Access is key to preventing escalation
The path from discovery to licensing a vaccine is not enough.
Vaccines only work when they are given to the people who need them. But, as the data shows, while it’s brilliant that the number of new vaccines being introduced in different countries is increasing, there is a long way to go. The underlying access issues must be addressed for existing vaccines. That way the full benefit and impact of these new vaccines can be felt by everyone – including the most vulnerable.
More needs to be done to make sure vaccines are easy to access and that people know how, when and why to get them.
This is not just essential for immunisations to address current infectious diseases but also for ensuring we have resilient infrastructure for the introduction of future vaccines like tuberculosis, dengue and respiratory syncytial virus (RSV).
There are also still research gaps that need filling to give us more robust evidence around what’s causing low coverage and the solutions for better predicting and preventing future escalation disease escalation. The gaps are often context specific.
This means working closely with those in the areas disproportionately affected and most vulnerable to future threats and bringing together expertise from a range of disciplines, keeping equitable access at the heart of everything we do.
What needs to happen now to improve vaccine coverage?
Fortunately, Immunisation Agenda 2030 (IA2030) offers a clear strategy and a committed global partnership whose mission is to tackle this crisis. Wellcome’s focus on escalating infectious disease means we shall continue to play our part too.
But, for us to succeed we need all governments, funders, civil society and wider immunisation partners to take the following collective action:
- Leverage political commitment, pandemic preparedness initiatives and current global health architecture strengthening efforts to ensure investment in key areas. For example, improving vaccine research and development, disease surveillance systems – and routine immunisation systems.
- Implement evidence-based, people-centred, and tailored strategies to build trust in vaccines and immunisation, counter misinformation and increase vaccine uptake particularly among vulnerable communities.
- Understand and test solutions to context-specific challenges for expanding vaccine services in underserved areas to reach missed children and vaccinate during outbreaks.
The time to act is now.
We’re funding research to better understand what causes and drives infectious diseases to escalate and the solutions to control their impact. Explore our current funding calls:
Infectious Disease Clinical Trial Award: Optimising interventions for impact