Episode 1: What can we do to stop superbugs?
After years of antibiotics being abused and overused, we now face a silent pandemic where the treatments we rely on no longer work. Dr Anand Anandkumar joins Alisha to correct the misconceptions around antimicrobial resistance and explain what we can do about it.
Listen to this episode
Speakers: Dr Anand Anandkumar, Alisha Wainwright, John Kariuki, Benard Wanyama
Alisha Wainwright 00:04
This is When Science Finds A Way: a podcast from Wellcome about the science that's changing the world. We hear so much in the news about the health challenges humans are up against: climate change, the global mental health crisis, disease outbreaks, the list is endless. And it's so easy to feel overwhelmed by it all. To be honest, it's easy to switch off. But this is where science comes in. Because there are people working all around the world at the cutting edge of scientific research. They're coming up with creative, often revolutionary solutions to our most pressing health challenges. And they're already having an impact at the local level with ideas that have global significance. Fascinating, right? I'm Alisha Wainwright. And now, I'm an actor living in Los Angeles. But in a previous life, I was one of those people doing science to try and understand the world better. I got my degree in botany, and worked as a field researcher in labs from the Panama Canal to the state of Colorado. And speaking from this experience, I know science is most powerful when it's diverse. That means diversity of ideas, and the kinds of people working on them. And that's what we'll be sharing with you here on When Science Finds A Way. You'll hear a truly global range of experts, scientists, researchers, people working at the forefront of scientific progress. And you'll hear from the people who have inspired and contributed to their work, people directly affected by the challenges we face. Sure, this stuff isn't easy, but there is hope. Science is helping to build a healthier future for all of us.
Oh, my, do we have a big one for you today? Antimicrobial resistance – AMR for short. It affects every single one of us on the planet. Yep. Even you. It's so pervasive, some call it the silent pandemic. And it's so misunderstood that most of us don't even know it's happening. I'm not gonna lie. When I first started doing research for this episode, I was genuinely horrified. People all over the world are dying from minor infections, infections that at a previous time could have been cured. And worse yet, it sounded like no one was trying to solve the problem. But before you rush and turn this off in despair, stick with me on this. The man you're about to hear from is a much needed ray of light. He's an engineer turned biotechnologist and his company, the awesomely named Bugworks, is trying to do something huge, that could literally change the world.
Dr Anand Anandkumar 03:06
This is why AMR is shaking the foundations of our society – because it's like oxygen. You'll never speak about oxygen every day, but it keeps you and me alive.
Alisha Wainwright 03:15
You'll also be hearing an incredible personal story about how AMR can play out in real life.
John Kariuki 03:22
But after five weeks, there was no improvement. I had to fight for my life.
Alisha Wainwright 03:28
It shocked me, it was inconceivable that this could be happening now, in 2023. And it made me realise how much I did not know or had misunderstood. So buckle up. It's a bumpy ride, but I promise it's worth it. Here's my conversation with Dr. Anand AnandAnandkumar. But don't tell him I called him that, he prefers Anand. And I started by asking him to give us an elevator pitch. What is AMR?
Dr Anand Anandkumar 04:00
Alicia, the simplest way of putting this is when existing antibiotics, antivirals, and antifungals stop working, because the bugs have simply mutated and have changed from what we believe them to be. That is antimicrobial resistance, when the organism is able to resist the very treatment that it's supposed to kill. That’s basically AMR. And it's in the news today, because we are losing the few antibiotics and antivirals that we have with us. And we have seen what COVID can do to damage lives and livelihoods. And we had that wake up call and several other wake up calls waiting to happen. So AMR is in vogue, unfortunately, and in the news because of what we have as humans done, which has caused these bugs to also become smarter and adapt faster.
Alisha Wainwright 04:55
Ooh, “what we as humans have done” – that sounds very ominous, and we'll get to that in a minute. But just before we do, can you start by giving me a sense of the breadth and scale of the problem?
Dr Anand Anandkumar 05:09
To make matters simple, let's focus on antibacterials. Because, Alicia, today when people say, AMR, they're specifically talking about bacteria that causes everything from urinary tract infection to abdominal infection, to pneumonia, to neonatal sepsis, head to toe infections, typically, people are talking about antibacterial issues. The scale is staggering. A report that came out in February 2022 said that 5 million deaths are attributable owing to AMR, anti-bacterial AMR, of which 1.5 million are directly caused by AMR. These numbers are growing by the year. Unfortunately, certain low to medium income countries face a brunt of this problem. And it's everywhere, because bugs have no passports. So a problem picked up in India or South African can show up in Glendale, or Montrose, Los Angeles by a single flight. So this is a huge problem. And a silent pandemic is just about to play on us.
Alisha Wainwright 06:20
Okay, I'm trying to be calm, but you're kind of reminding me of when I first learned about climate change and global warming. It's this sort of looming sort of monster in the distance that you can't quite grasp. So I just want to know, how did we get here?
Dr Anand Anandkumar 06:35
So if you go back in time, 1920s, about 100 years ago, Alicia, that's when penicillin was found. We only have a 100-year history with antibiotics. And as and when new antibiotics started happening, bacteria started developing intelligence, evolutionary intelligence and resistance to these antibiotics. Number two, antibiotics is not a very remunerative area compared to cancer or cardiovascular diabetes. So there's less innovation happening, low pricing, people are just not interested in the space. So look at the perfect storm we have created a globally mobile audience, massive use an abuse of antibiotics, no innovation.
Alisha Wainwright 07:20
With the massive use, when they first created antibiotics, did they know that there was an opportunity for there to be resistance in the bacteria?
Dr Anand Anandkumar 07:30
Alexander Fleming, who won the Nobel Prize for inventing antibiotics, in his Nobel Prize acceptance speech, said, yeah, while you're appreciating my work, I'm sorry to tell you that bugs are smarter than us. They've had millions of years of evolution, they’re going to pickup – please use penicillin with care. Don't abuse it. Alexander Fleming said this in the 1940s, if I'm not mistaken, so we knew it. But the rate of resistance pickup is happening much faster than it happened in the 1950s, 60s, 70s. Because we're using billions and billions of antibiotics for humans, we're using billions of antibiotics for cattle, for the meat industry, and climate change exacerbates this problem. So in the last 30 years, we have exacerbated something that was always there. But it's become much worse very quickly.
Alisha Wainwright 08:22
Okay, so it's in our healthcare system. It's how we keep our animals. It's how we farm, it's our environment. It's everything basically.
Dr Anand Anandkumar 08:30
Exactly right. Which is why AMR is like a climate problem. And it's called a one health issue, because it impacts humans, animals and environment in a very tight loop.
Alisha Wainwright 08:43
And I'm keen to know your personal relationship with this issue. And India is a hotspot for AMR. So I'm curious, how did it come up in your family when you were growing up? Was your family one to kind of just immediately go to the doctor for antibiotics?
Dr Anand Anandkumar 08:58
My father was a very famous doctor in India. He practiced for 53 years before he passed away, very vaunted physician, and he treated tuberculosis for many decades. So I grew up in a family that's filled with doctors, and lines of patients around my house with TB. And then in the 1980s, it was my father who attended the first HIV patient in India. So the family has a history with infection. I grew up knowing to treat antibiotics with great care, never to take antibiotics without my father's prescription, to always complete a full course of antibiotics, never to split the tablet into two. But I was an engineer, right?
Alisha Wainwright 09:38
You were born to do this!
Dr Anand Anandkumar 09:40
Exactly Alisha. I'm an engineer. I'm not a doctor. I'm not a scientist. It's in my late 40s that I understood the purpose of my life and changed from engineering into biotech, but it looks like the subconscious in me took over in my late 40s to want to do an anti-bacterial company.
Alisha Wainwright 10:01
Right, okay, so you are totally immersed in the field of AMR, but, you know, what about everyone else? Do you think that people really understand the scale of the problem?
Dr Anand Anandkumar 10:11
AMR is just like climate. We know it's out there. There's no one owner for it. It's caused by multiple problems. Right now, in the last two to three years, we realise that it can completely shake humanity. So slowly, we're waking up to this reality. Unlike climate, AMR, you don't see it. It's quietly happening in our cities, quietly happening in the suburbs, quietly happening all over the world. And by the time we wake up to this reality, it may be too late.
Alisha Wainwright 10:40
So I guess just to ask the question in a different way, because I'm curious, like, when you meet people, and – I don't know how often you're bringing up AMR at the dinner table – are you noticing clear misconceptions from the general public?
Dr Anand Anandkumar 10:57
Yes, I do. Because there is no appreciation of the difference between antiviral and antibacterial. It all starts from there. Even in the United States, a very large percentage of antibiotics used are for infections that are not caused by bacteria. Antibiotics can only work when you have proof that the infection is directly related to a bacteria that has caused it, right? You do a sensitivity analysis, and you say bug A, or bug C has caused it. And this antibiotic should work on bug A or C, you prescribe it. In many cases, we don't go and do a diagnostic test, and we start using an antibiotic each time you use an antibiotic when it's not needed, you're perpetuating AMR.
Alisha Wainwright 11:43
Okay, hold that thought because we wanted to put this into real life context. We're going to hear John's story. He's a veterinary surgeon from Kenya. So he definitely has a higher than average knowledge of AMR. Back in 2020, he had a nasty fall in the shower, he had to have surgery to insert some metal plates to heal the break. But that was the beginning of an even more horrible journey with AMR.
John Kariuki 12:10
After I had the operation, the surgical wound continued swelling, and it started discharging, despite me using the prescribed antibiotics during that time. And it got so bad that it triggered high blood sugar. And this actually drove me into a semi coma. And then I had to undergo another surgery to remove the metal plates. Because the infection had gotten into the blood, I had become what you call septicemic. One time, I called my wife aside, and I told her, the way I'm feeling now, I think I've reached the end, please, take care of yourself, take care of the the family. Probably we will meet again, in heaven. I never got better. The COVID-19 infection that came during that time did not make things any better. I had to fight for my life. And then after five months in hospital, I was released to go home. Still very dilapidated and debilitated. Very weak. I could hardly stand, I had to be helped to bed, to the wheelchair. Actually, when I was released from hospital, the wound dresser came home with me. And he visited me twice a week and did the dressing of the wound. But after five weeks, there was no improvement. And when I thought about it, is when I decided to do cultural sensitivity testing and get the results for myself and get to know what is going on. Thank God I had a background in pharmacology, toxicology and medicine. I got the results that showed an organism that was causing the problem. A bacteria called a citrobacter. Eighteen antibiotics had been tested on it, and only one antibiotic, called Amikacin, was working. And so I went ahead and had Amikacin administered for five days. And after about three weeks, the wound started drying up, and that is how I recovered. My hospital bill came to around thirty-five thousand US dollars. I spent another ten thousand dollars at home. And then the drug that was working cost less than, maybe, fifty dollars – less than fifty dollars. Following the surgical manoeuvres and the problems I had in hospital, my leg is now three inches shorter, and I’m actually registered with the Kenyan government as a person living with a permanent disability. This, to me, was unthinkable before, but I'm having to cope with it, and I'm happy to prefer to live with it, rather than have other surgical manoeuvres done, and expose me to another round of antimicrobial resistance, and sickness, and recovery, and complications that may come with it.
Alisha Wainwright 15:36
I cannot believe that if he hadn't thought to do a sensitivity test, he could have been one of those millions of people that succumb to AMR.
Dr Anand Anandkumar 15:46
Absolutely. It's an incredible story, very moving. And this type of story can now happen anytime, anywhere. It can be China, it can be India, it can be the United States, it can be the UK. You know, seriously, bugs have no borders. Number two, the gentleman spoke about doing a sensitivity analysis and one of the drugs Amikacin was sensitive. Guess what? It's produced only by a handful of companies all over the world, because it's not a regularly used drug. So you somehow have to pray and hope that the supply chain of these rare drugs are available in your country. So this is really, really scary. And the third thing is the entire modern medicine, surgery, oncology, chemotherapy, hip replacements are all based on antibiotics working successfully. The best surgeons in the world will do their job and when she or he is gone, a patient may pick up an infection that's untreatable. This is why AMR is shaking the foundations of our society, because we depend on it. It's like oxygen, you never speak about oxygen every day, but it keeps you and me alive. It's antibiotics that keep the edifice of modern medicine going. And that very edifice is cracking.
Alisha Wainwright 17:05
And to your point, do you think that the antibiotic Amikacin would even work today for him if he had the same situation?
Dr Anand Anandkumar 17:12
Don't know. In many parts of India, Amikacin is completely useless. So in fact, I'm pleasantly surprised it worked for the gentleman, and I'm happy it did. But the similar infection in his neighbourhood may not work for Amikacin, because it's so personalised, and the bugs are mutating so quickly. So the answer is, you don't know.
Alisha Wainwright 17:32
Something he said at the very end kind of upset me too, because he was basically not wanting to do further corrective surgery, which would benefit his own health ,in order to potentially, you know, remove the option of getting another infection.
Dr Anand Anandkumar 17:46
Yeah, so there are many parts of the world today, where unless it's absolutely necessary, they don't want to do a surgery because they're worried about post-surgical infection. Can you believe this? In 2023, I'm making this comment. And this is starting to,increasingly, from parts of the world where I come from, they’re really worried. And for your audience, I must also let you know that 20% of all people who die, post cancer therapy, post chemotherapy, are not dying because of the cancer, but are dying because of infection that they pick up post chemotherapy. Because when you have an oncology treatment, or a diabetes treatment, or rheumatoid arthritis treatment, your immune systems are suppressed – perfect environment for bacteria to get in.
Alisha Wainwright 18:32
Wow, I did not know that. That is a very sobering thought. But before we get too depressed, there is important work being done around the world to try and prevent the ordeal that people like John went through.
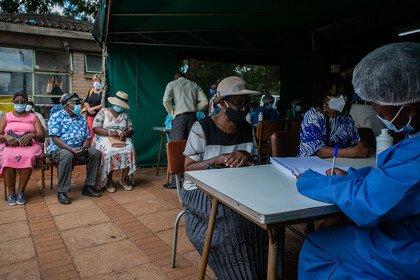
This is Kakamega Hospital in Kenya. Alongside a handful of other hospitals in Ghana, Malawi and Uganda, it has been part of a surveillance project since 2020, which is aiming to better understand the burden of antimicrobial resistance on patients living in low and middle income countries. It's called and this is an acronym, SPIDAAR – “speeder”, “spider”, pick your poison. It's short for Surveillance Partnership to Improve Data for Action on Antimicrobial Resistance. Did you get that? Okay, great. Samples from sick patients are sent off for sensitivity testing, and the data is analysed and shared across the four countries. As well as providing big picture data on resistance patterns in the region. It's also proving to be a game changer when treating patients. We caught up with Benard, an infectious disease pharmacist in the hospital, to find out more about how the project has changed his work.
Benard Wanyama 19:55
Since the SPIDAAR project started, so much has changed. The level of understanding of antimicrobial resistance and microbial stewardship has really gone up. We are now able to cut out a number of tests that support the doctors to be able to make clinical decisions. And this is not just in terms of doctors and other health care workers, even the patients, they are happy because we are able to make timely interventions and be able to give the right or appropriate antibiotic. We had a baby in the newborn unit whose fevers were just going up, despite the fact that there were very good antibiotics. So we struggled, and eventually we got some blood, we go to the lab, we were able to do a culture. And actually it was a mixed growth. So what we did, we were able to introduce new antibiotics to this newborn. And actually, the baby responded, so that eventually, they came out of the newborn unit. So it was a big thing. Remember, she spent a lot of time, more than three months in the newborn unit. So the mother was so happy. So that is a case that I think it's taught us a lot. Because sometimes there are some bacteria, we feel that they are just normal flora, they don't cause any infection. But you will have to interpret results in relation to the state of the patient. So we believe we are making a difference. Previously, you come to work, and you don't have the tools to support you to be able to do what you learned in college. So it used to be very frustrating, very, very frustrating. But because we are able to adequately diagnose, then, you wake up in the morning, at least you have the passion to go to work, because you know you will make a difference in someone's life.
Alisha Wainwright 22:06
Ah, wow. What gets me about that is, kind of going to the point of doctors doing their work and then letting the rest of the system sort of play out. And if your patients keep dying from antibiotic-resistant infections – your work, how do you get up and go to work every day, if you know that your patients are dying from this?
Dr Anand Anandkumar 22:29
That's right, you may be the most talented doctor, clinician or surgeon, but a resistant bacterial infection is out of your hand if you don't have the tools to deal with it, right?
Alisha Wainwright 22:39
Right, of course. But what gives me hope is to see that positive change is happening with research projects like this, and actually, you know, Benard told us that alongside improving their antimicrobial stewardship in the hospital, one of the big learnings for the whole team was around basic hygiene standards that needed to improve, which is another really important AMR prevention tool.
Dr Anand Anandkumar 23:05
So if you look at some of the best returns we have had in the last 10 years, with spending least amount of money, it's in WASH – water and sanitation hygiene. Again, COVID taught us that using masks sanitising our hands etc., did a lot to prevent even worse COVID spread. So most hospitals we look at in India, Africa, Southeast Asia, LatAm, the hospitals are much better. The last 10 years we've made significant progress. Is there room for improvement? You bet, there's plenty of room for improvement. But we have come a long way. And we find that hospital-acquired infection can be somewhat contained by simply following good hand hygiene, because in hospital-acquired infection, one patient is not infecting the other patient. The patient's bugs are carried by the nurse or the doctor or the caretaker who touch the surface or the patient herself or himself, and then move on to the next patient, or the surface that the next patient touches. So it's these healthcare workers that are spreading the hospital-acquired infection.
Alisha Wainwright 24:13
Wow, that's reassuring because I feel like it's something everybody can do.
Dr Anand Anandkumar 24:17
Absolutely.
Alisha Wainwright 24:26
So we've looked at some of the ways we can slow down the advance of AMR. But now the big question, what happens if we run out of antibiotics? I mean, are we going to go back to a pre-penicillin era where people were dying from something as simple as scratch?
Dr Anand Anandkumar 24:42
So, I'm going to be very careful how I answer this because people may think that since I work in the area, that we may be potentially exaggerating. So I'll pull back, I’ll be careful but I'll state the fact: if the pipeline of how we're creating new antibiotics, antibacterials does not improve and improve quickly, I'm afraid we will be left to deal with last-resort situations. That means: patient comes in, he or she has pricked their hand or a small surgical incision, picked up an infection, and the antibiotics available in that hospital are not enough to treat the bug. This pandemic is a silent pandemic. COVID was not a silent pandemic, it's in your face, massive spread, spikes and come out quickly etc. AMR spreads quietly. In fact, many deaths in the hospitals don't even get recorded as an AMR death, they'd say kidney failure, or cardiovascular failure, therefore, the numbers you're hearing are grossly under-counted. So if you don't do serious things about saving existing antibiotics, and investing in a new generation of antibiotics and treating it like medical infrastructure, not as a business, we will move to a pre-penicillin era. And then even if you came and gave me one billion, two billion, three bullion, I can't produce an antibiotic overnight. It takes ten to twelve years, at a minimum, to do an antibiotic, if at all, you're successful, and a billion dollars. Which pharma company wants to spend a billion dollars and then tell you, Alicia, don't use my drug, keep it carefully under lock and key? And when the doctor says, “it's a tough case, only for that case, when you've proven it through a sensitivity analysis, use my antibiotic” – it makes no sense from a business perspective.
Alisha Wainwright 26:35
So, in short, you know, you'd have to be crazy to take this on. And that's where you come in. Your company is one of only a handful globally that's attempting to come up with a broad spectrum antibiotic. So please, please, please tell us more.
Dr Anand Anandkumar 26:50
So Bugworks... I hope you like the name, it’s a cool name.
Alisha Wainwright 26:54
It is a cool name.
Dr Anand Anandkumar 26:51
Initially my scientist thought, like, “what is this, like, a cartoon character?”, but now it's caught on. Bugworks was started ten years ago, I spun this company out of my previous company called Cellworks. And ten years ago, we started seeing the writing on the wall sitting in India. I'm a US citizen, but I sit in India. And we started seeing too many people dying, babies dying of neonatal sepsis, no pharmaceutical company showing interest. And we said, “huh, what if we can put a company together that creates a completely new generation of broad spectrum, with trying to invent the first novel, broad spectrum antibiotic since the 1960s?” I was born in the 1960s. The last novel class was called fluoroquinolones. And since then, there has not been a completely novel class of broad spectrum.
Alisha Wainwright 27:45
For someone who doesn't know, in the simplest term, what is a broad spectrum antibiotic?
Dr Anand Anandkumar 27:50
A broad spectrum antibiotic is one that hits a target in a bacteria. And that target is preserved across many bacteria. So a single shot or a single drug, like the fluoroquinolones, it can help you for multiple infections. Therefore, our solution can potentially work on many infections. That's called a broad spectrum. Typically, you don't use a broad spectrum for everything, you use it for bad patients, when you're not sure what the hell is going on. Patient is going down quickly, you need a broad solution because you think it's multiple bacteria causing problems and let's just kill everything, heal everything, stabilise the patient in two days, three days and then move to a step down treatment, right? So you need a step down. But you first you need to start here. So our broad spectrum works on a whole host of organisms that cause meningitis to skin infections to urinary tract infection to pneumonia, to abdominal infection, sexually transmitted diseases, cystic fibrosis, which is a big problem in the United States and UK for the Caucasian population. And we also work on bacteria that causes bioterrorism. So we have an application in public health, and we have an application in bio-defense.
Alisha Wainwright 29:09
Like anthrax?
Dr Anand Anandkumar 29:10
Like anthrax, like bubonic plague, and many more things I can’t speak about that are either naturally occurring or potentially engineered by some operators, we won’t speak about where they could come from. So we are potentially – we're not the only company but one of a handful of companies working on a single stop solution for public health and biodefense.
Alisha Wainwright 29:32
Jeez. Okay, wow. So just a small aim for your company then. But you know, how close are you to actually making this reality?
Dr Anand Anandkumar 29:42
We have cracked the superbug in pre-clinical. That means our novel antibiotic is entering these superbugs, hitting the superbugs in new targets, novel targets and causing quick death to these bacteria, so that they can't mutate that quickly. Bacteria will defeat us. But a new asset like ours could give a twenty-five, thirty year period for humanity to figure out other solutions. Never permanent. But you give adequate time.
Alisha Wainwright 30:13
Because it's constantly evolving.
Dr Anand Anandkumar 30:16
And much more intelligent than us, much more intelligent. As we have completed our preclinical studies, and phase one clinical trials are running in Australia. Wish us luck, because if our phase one succeeds this year, we have a big new asset for humanity. It has been tested on ten thousand superbugs across the universe. And it seems to have a fantastic efficacy. But I cannot claim success until we complete the early clinical trials and know that the safety of the product is adequate.
Alisha Wainwright 30:48
But you're hopeful.
Dr Anand Anandkumar 30:50
Hopeful, and the early signs that you're seeing show that this thing, the risk to reward equation is very much in our favour.
Alisha Wainwright 31:00
Wow, that is broad spectrum. That's truly fascinating. Okay, so if the business case isn't there for developing these broad spectrum antibiotics, what should governments and the scientific community be doing to stop the globe from getting to the point of no return?
Dr Anand Anandkumar 31:21
Since the return on investment is so poor in antibiotics, because there's no volume, governments are starting to look at antibodies like defence infrastructure. When you have that warship that's parked near Los Angeles in a port, you really don't care about how many times you're using it. In fact, you hope you never use it. But it's there for you, and your tax dollars have somehow funded the Department of Defence to put that warship there, correct?
Alisha Wainwright 31:48
Yeah, that's a really smart analogy.
Dr Anand Anandkumar 31:52
If you have a fire extinguisher in your house, I pray and hope nobody ever has to use one. But if a bad occurrence happens, you have a fire extinguisher but you still pay for it. You pay for your fire insurance, you keep it and we pray and hope you never use it. So people are thinking about antibiotics like fire insurance or defence insurance and say, don't treat it like a cholesterol drug. Don't treat it like a blood pressure drug, where you can sell hundreds of millions, right? Keep it. So society is able to go on with its medical practice, don't worry about volume. So decoupling volume from value. And the United States and the UK are leading this discussion by saying, “let's put money on the table. So if a company's able to crack the superbug and get a drug that works for your public, we will keep it under lock and key.”
Alisha Wainwright 32:44
And your warships?
Dr. Anand Anandkumar 32:45
And your warships, right. And you never look at how many bombs were ever fired from that stealth fighter. So unless antibiotics are treated like a global infrastructure, that becomes a very lifeline of modern medicine, this space is game over.
Alisha Wainwright 33:05
Well, if anyone else that's listening feels like how I'm feeling, I'm feeling a little stressed. I don't love the idea that not enough is being done to curb this incredibly important global issue. So, I need you to give me a pep talk. What can I be looking forward to? How can I feel better about this?
Dr Anand Anandkumar 33:26
Lots of good things have happened in the last four to five years because we were in such a desperate situation. I want to appreciate the Department of Health and Human Services of the United States, the Wellcome Trust, Bill and Melinda Gates Foundation, WHO, etcetera, for putting some money on the table to fund what I'd like to call “push” incentives. That means you're pushing innovation, small struggling companies like mine, get some grants to work on science. This wasn't the case, five, six years ago. So good news for the audience is, there is hope. Point number two, grants are slowly starting to creep up to fund clinical development, which is the expensive part. Here again, governments like the US, UK, Australia, Canada, etcetera, are doing a lot of work. Governments are also starting to write laws, they want to pass laws that are going to put some money on the table to say, “please support companies doing innovation in antibacterial so they can stay alive with the lights on”. So I see lots of things happening, which give me hope. If the business side of things does not get fixed in anti-infectives, we will still have a problem. But I see some change coming. And the next time we meet I hope to give you even more, better updates. But it's not hopeless.
Alisha Wainwright 34:43
Okay, and if you have hope and you're on the frontlines, then I have hope and I'm also wondering, in my day to day life, what can I do to help the situation if anything?
Dr Anand Anandkumar 34:57
Yes, you can. As they say, a journey of a thousand miles begins with the first step. You fall sick, you're feeling sick, you're having a fever: please don't take an antibiotic, unless your doctor asks you to do it and you have a proven bacterial infection. Basic hand hygiene, wash your hands, WASH: the basic discipline goes a long way in preventing the spread of AMR. If possible, please buy meat, chicken, etcetera, that is certified not to be treated with antibiotics. In the developed parts of the world, the biggest culprit of AMR is the use of antibiotics in your protein. In the developing parts of the world, it’s easy access and use and abuse by humans that's causing it, so it's very interesting. In one part of the world, it's humans, just popping antibiotics. Just like you know, chocolate. In one part of the world is your craze for animal protein, and the food chain that's exacerbating this problem.
Alisha Wainwright 36:01
Well, Anand, you are making your mark on the world, and I look forward to seeing what the clinical trials will reveal, and hopefully, your broad spectrum antibiotic will save many, many, many lives.
Dr Anand Anandkumar 36:12
Thank you so much, Alicia. I thank you and the Wellcome Trust.
Alisha Wainwright 36:18
Thanks for listening to this episode of When Science Finds A Way. And thanks to Dr. Anand Anandkumar and our contributors John Kariuki and Bernard Wanyama. I know AMR sounds scary, but it does give me hope that people like Anand and Benard are working on it.
When Science Finds A Way is brought to you by Welcome. If you visit their website, wellcome.org, with two l's you'll find a whole host of information about AMR, as well as full transcripts of all of our episodes. Make sure you follow us in your podcast app to get new episodes as soon as they come out. And if you feel like you learned something important or interesting, or you just want to support the podcast, spread the word and share it with people you know. Next time we'll be hearing how research into new family forms has transformed the quality of life for same-sex parents and their children.
When Science Finds A Way is a Chalk and Blade production for Wellcome, a global charitable foundation that supports science to solve the urgent health issues facing everyone.
Show notes
Since the discovery of penicillin in the early 20th century, we’ve seen the risk of minor infections virtually disappear. But after years of antibiotics being abused and overused, we now face a silent pandemic where the treatments we rely on no longer work.
The potential scale of antimicrobial resistance, or AMR, is staggering, and there is a lack of awareness of just how dangerous it could be.
Alisha speaks to Dr Anand Anandkumar, an engineer turned biotechnologist, to correct the misconceptions around AMR, and discover what we can do about it. We’ll also hear from John Kariuki in Kenya, whose own experience with AMR almost cost him his life, and Benard Wanyama, whose project is treating patients with infections and monitoring the spread of AMR.
Together, they make a powerful case for urgent and collective action to stem the tide of superbugs.
Meet the guest
Next episode
In the 1970s, when a heterosexual couple divorced, courts almost always awarded child custody to the mother, except in one scenario: when the mother had come out as a lesbian. Professor Susan Golombok joins Alisha to discuss how her research has since changed laws and perceptions on same-sex parenting.
Transcripts are available for all episodes.

More from When Science Finds a Way

When Science Finds a Way: Our podcast
Our podcast is back with a third season, uncovering more incredible stories of how scientists and communities are tackling the urgent health challenges of our time.