Why is a global Covid-19 vaccine rollout vital?
Read more about what's at risk if countries do not share their excess doses and ensure an equitable global rollout.
The Covid-19 pandemic doesn't end with a vaccine. It ends when everyone can get it.
Covid-19 vaccination efforts are picking up worldwide, bringing hopes of returning to a more normal life. But nearly half – 48% – of all vaccine doses administered so far have gone to high-income countries, making up just 16% of the world's population and leaving large parts of the global population unprotected. This imbalance puts us all at risk. Our best defence is to work together and ensure all countries have access to Covid-19 vaccines.

UNICEF/2021
COVAX-supported Covid-19 vaccines arriving in Nicaragua in March 2021.
Rich countries that have secured lots of excess doses must donate these through COVAX, who will ensure that vaccines go where they are needed most.
So, who currently has access to Covid-19 vaccines? Are countries sharing their excess doses? And, how can these countries ensure that those who need vaccines get them?
Countries around the world have bought 8.9 billion Covid-19 vaccines.
But high-income countries have made the majority of these purchases.
Several countries have ordered far more vaccines than they need. Governments in high-income countries have purchased 56% of the world’s Covid-19 vaccine supply, despite representing just 16% of the global population.
And inequality in vaccine procurement has led to inequality in vaccination rollout. For example, just 1% of the 100m vaccine doses administered between 19 to 24 April went to people in low-income countries.
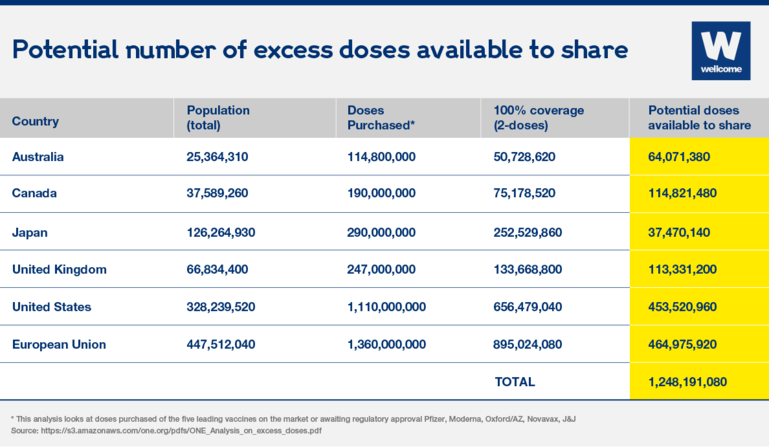
The UK, US, EU, Japan, Australia and Canada (among others) have bought more doses than would be needed to vaccinate their entire populations. Between these five countries and the EU bloc there are over 1 billion surplus doses of the five leading vaccines (Oxford-AstraZeneca, Pfizer-BioNTech, Moderna, Novavax and Johnson & Johnson) available, enough to vaccinate all the vulnerable groups (healthcare workers, people over the age of 65 and people with underlying health conditions) in every country around the world.
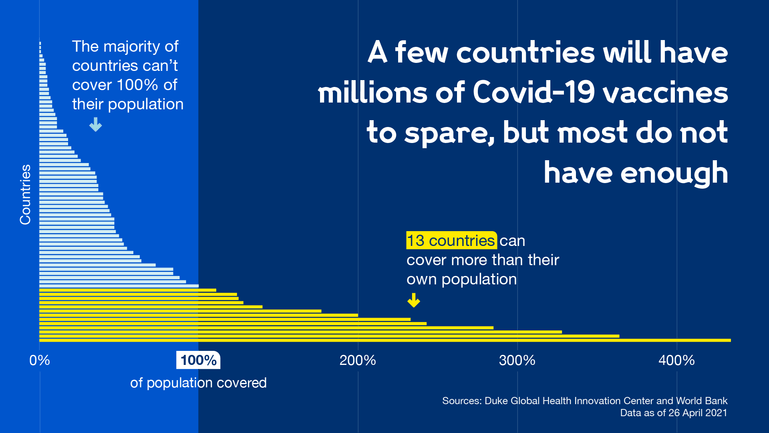
13 countries have enough Covid-19 vaccines to cover their population multiple times, while the majority of countries do not have access to enough doses to cover 100% of their population.
Data from Duke Global Health Innovation Center and World Bank. Data is accurate as of 26 April 2021.
Not all these doses have yet been manufactured and delivered, but as they have been pre-ordered, vaccine producers are committed to supplying them.
Overall, the available global manufacturing supply for this year is spoken for, so low-income countries cannot now buy more doses. So, the best and fastest way to achieve a more equitable distribution of vaccines lies in the hands of countries that have ordered more doses than they need. They can do this by sharing doses now through COVAX, in parallel to their own national vaccine rollouts.

Read more about what's at risk if countries do not share their excess doses and ensure an equitable global rollout.
24 million doses have already been shared by countries directly through bilateral deals between one country and another. Of those, over half have been from China.
27 million vaccines have already been donated by countries directly
90% of which have come from China and India. But not through COVAX.
Health officials and advocacy groups have highlighted these bilateral deals risk creating a chaotic situation where public health considerations are sometimes not the main driver.
To ensure that vulnerable groups around the world have access to vaccines, it is crucial that we take a coordinated approach through COVAX, rather than use lots of piecemeal individual agreements. This will ensure efficient and equitable targeting of doses based on local need and capacity.
Here are 3 reasons why...
COVAX was built with global equity at its heart. Donations outside of COVAX risk a fracturing of the global response, with health needs potentially taking second place to the political objectives of individual governments. This could leave vulnerable populations around the world locked out of access to vaccines. COVAX operates in line with the World Health Organization Allocation Framework, so donated vaccines will go where they are needed most.
Sending vaccine doses between countries involves huge complexity. There are regional and national regulations to comply with, as well as delivery and storage needs for the different vaccines such as extreme cold chain for Pfizer-BioNTech doses. COVAX assesses which countries are ready to receive which vaccines, ensuring they are used most effectively. This reduces the risk of vaccines being wasted or delayed in their use due to incompatibility with recipients’ infrastructure.
Any doses procured through COVAX would be quality assured and would be covered by all the legal provisions such as indemnity and liability, including the no fault compensation scheme.
COVAX hopes to deliver more than two billion doses to people in 190 countries in less than a year, but it needs urgent funding to meet those goals and for countries with surplus vaccines to donate them now.
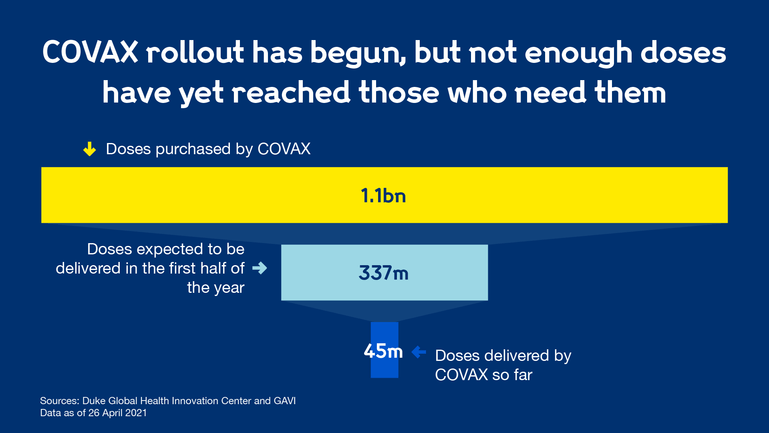
COVAX has purchased 1.1 billion Covid-19 vaccines, and expect to deliver 337 million of these in the first half of 2021. As of 26 April 2021, COVAX has delivered 45 million Covid-19 vaccines.
Data from Duke Global Health Innovation Center and GAVI. Data is accurate as of 26 April 2021.
To safeguard our hard-won progress towards ending the pandemic, we need urgent international action to achieve more equitable global access to vaccines.
This article was first published on 26 March 2021.


