Act now, act together to end Covid-19
As global efforts continue to make sure Covid-19 tests, treatments and vaccines are available to those who need them the most, Will Hall writes about the ACT-Accelerator and the importance of a coordinated global response, delivered locally.
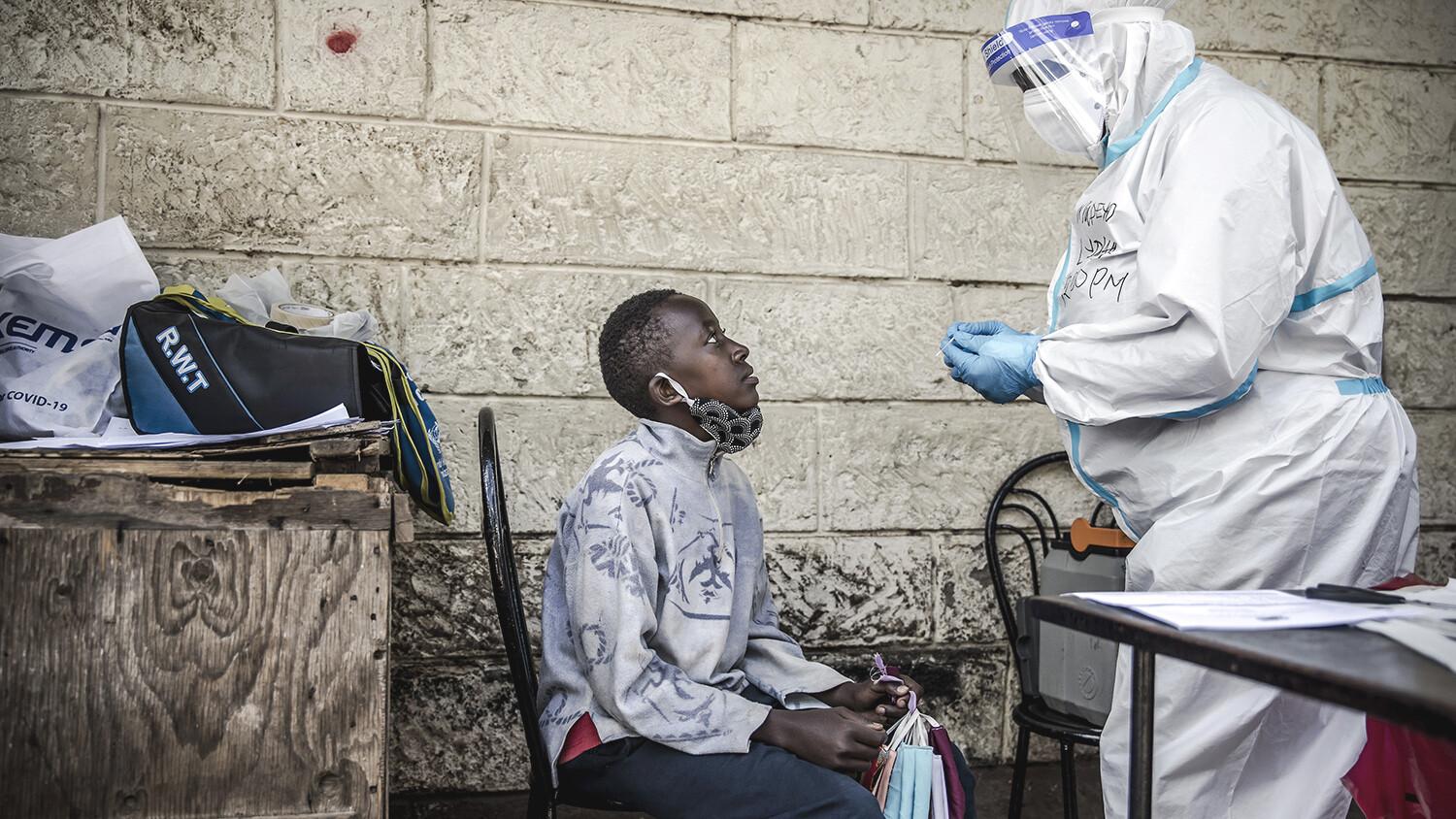
Six months after the first coronavirus case, we can see the catastrophic effects that Covid-19 has had on societies and economies across the world and the scale of what will be needed to get us out of the crisis.
More than half a million people have already lost their lives and all countries remain vulnerable to current or future outbreaks. As lockdowns and social distancing begin to ease, time is not on our side to get the lifesaving solutions to test, treat and prevent Covid-19 to those who need them the most.
In March 2020, the Global Preparedness Monitoring Board called for $8 billion of financing to support the urgent development and distribution of tests, treatments and vaccines. Now Covid-19 has reached every corner of the world, global demand for these will be huge. But when and if these tools are found, the debate about making them available, affordable and allocated in an equitable way will intensify.
The COVID-19 Health Funding Tracker
The Economist Intelligence Unit’s COVID-19 Health Funding Tracker synthesises global, health-related funding efforts, from pledge to disbursement.
It tracks the flow of money towards development, production and equitable access to new COVID-19 diagnostics, therapeutics and vaccines, including those under the Access to COVID-19 Tools (ACT) Accelerator initiative, and relevant funding for health systems. The tracker will help increase accountability through greater transparency and target further pledges towards critical funding gaps.
What is the ACT-Accelerator?
In May 2020, governments, global health organisations, scientists, businesses, civil society and philanthropies came together to create the Access to Covid-19 Tools (ACT) Accelerator. This is a global collaboration to get lifesaving tests, treatments and vaccines from the laboratory to the front line.
Organisations from across global health are leading four pillars, focusing on research, manufacturing, procurement, equitable allocation and distribution.
Their aims are ambitious but essential:
- Diagnostics – to reach 500 million people in low- and middle-income countries with simple, affordable, high-quality and rapid tests to detect infection and contain the spread of the disease by mid-2021.
- Therapeutics – to develop, manufacture, procure and distribute 245 million effective treatments by mid-2021 in low- and middle-income countries.
- Vaccines – to speed up the search for an effective vaccine for all countries; at the same time, to support the building of manufacturing capabilities, and buying of supply ahead of time, so that 2 billion doses can be distributed fairly in the places of greatest need by the end of 2021.
- Health systems – to make sure that these tools can reach the people who need them most.
How much funding is needed?
Several billion dollars have already been raised to support this work, but more is urgently needed over the coming year. $3.4 billion has so far been pledged, and an additional $27.9 billion is needed.
While this funding is significant, it is a great investment to end the pandemic. It represents less than a tenth of the $37 billion the global economy is currently losing every month due to Covid-19, and it is only a fraction of the domestic responses major governments are mobilising to support their economies.
As international travel resumes once again, we are seeing that as long as Covid-19 is a threat somewhere, it is a threat everywhere. To stop the outbreaks, save lives and rebuild our economies we must provide the tools where they are needed most.
